Waking up at 3am and staring at the ceiling is one of the most common (and frustrating) menopause complaints I hear. You might fall asleep just fine, then suddenly your eyes ping open, your mind starts whirring, you feel too hot, or you get that “wide awake for no reason” feeling.
The good news is that this pattern usually has a few very explainable drivers in perimenopause and menopause, and once you know what they are, you can start making small changes that genuinely help.
“Why do I keep waking up at 3am during menopause?”
In menopause, sleep tends to become lighter and more easily disrupted. That is partly due to hormonal changes, and partly due to knock-on effects on stress hormones, temperature control, mood, and blood sugar.
A quick reassurance first: waking briefly during the night is normal. The problem is when you wake and cannot get back to sleep, or when it happens so often you feel exhausted, anxious about bedtime, or start relying on caffeine just to function.
The menopause sleep shift (in plain English)
As oestrogen and progesterone fluctuate (and then decline), your brain and body can become more sensitive to disruption.
- Progesterone has a naturally calming, “sedating” effect for many women. When levels drop, you may feel less settled at night.
- Oestrogen supports temperature regulation and can influence serotonin and other brain chemicals involved in sleep. Lower oestrogen can mean more night sweats, hot flushes, and mood changes that disturb sleep.
For a helpful overview of menopause symptoms and support options, the NHS menopause guidance is a solid starting point.
The most common reasons you wake at 3am (and how to tell which is yours)
3am is not a magical number, but it often lines up with predictable body rhythms, especially cortisol (your main “get up and go” stress hormone) starting to rise in the second half of the night.
Here are the big drivers I see in practice.
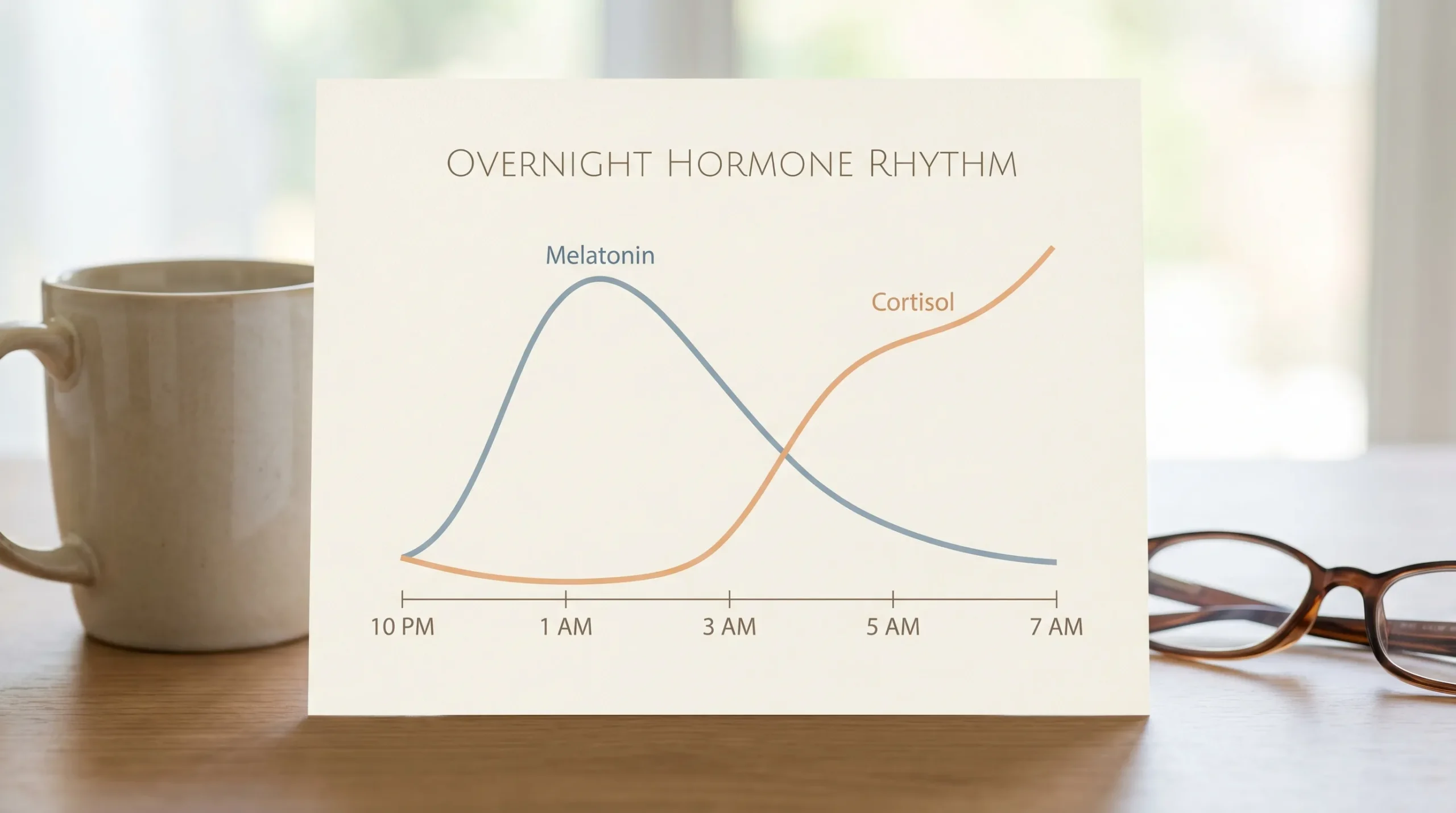
1) Cortisol is running the show
In a healthy rhythm, cortisol is low at night and rises towards morning to help you wake up. In perimenopause and menopause, cortisol patterns can become more “spiky” due to life stress, depleted resilience, blood sugar swings, overtraining, under-eating, or simply the hormonal transition itself.
Clues this might be you:
- You wake with a racing mind or anxious feeling
- Your body feels “wired but tired”
- You often wake at the same time each night
- You feel more tired in the afternoon, then get a second wind late evening
2) Blood sugar dips overnight
This one is hugely underestimated. If your evening meal is light on protein, fibre, and healthy fats (or if dinner is early and you are genuinely hungry), your blood sugar can dip in the night. Your body may respond by releasing stress hormones (including cortisol and adrenaline) to bring blood sugar back up. The result is that sudden 3am wake-up.
Clues:
- You wake hungry, shaky, or with a “buzzing” feeling
- You fall back asleep more easily after a small snack
- You are craving sugar/carbs mid-morning
3) Night sweats or temperature swings
Even if you do not fully wake due to a hot flush, temperature changes can pull you into lighter sleep and make waking more likely.
Clues:
- You wake hot, damp, or throwing covers on and off
- Sleep is worse after alcohol, spicy meals, or a warm bedroom
4) Alcohol, caffeine, and the “sleep quality trap”
Alcohol can help you feel sleepy initially, but it tends to fragment sleep later in the night. Caffeine can also linger longer than you think, especially in midlife.
Clues:
- 3am waking is worse after wine, late meals out, or afternoon coffee
- You fall asleep fast but cannot stay asleep
5) Low mood, worry, and perimenopause anxiety
Hormonal changes can increase anxiety for some women, and poor sleep then makes anxiety worse. This can become a loop.
If this feels familiar, it may help to know that evidence-based approaches like CBT for insomnia are recommended for persistent insomnia (your GP can advise, and the NHS has resources).
6) Other health factors worth checking
Sometimes there is more going on, and it is important not to blame everything on menopause.
Consider chatting with your GP if sleep has changed dramatically, especially if you have:
- Loud snoring, gasping, or extreme daytime sleepiness (possible sleep apnoea)
- New palpitations, breathlessness, or chest pain
- Symptoms of thyroid imbalance
- Low mood, persistent anxiety, or panic
A practical “3am wake-up” checklist (start here)
If you want a simple starting point, try these four foundations first. They are not glamorous, but they are powerful.
1) Build a more sleep-supportive evening meal
Aim for a dinner that contains:
- Protein (chicken, fish, eggs, tofu, lentils, Greek yoghurt)
- Fibre-rich carbs (new potatoes with skins, brown rice, quinoa, beans, oats, wholegrain sourdough)
- Colour (at least 2 different vegetables)
- Healthy fats (olive oil, avocado, nuts, seeds)
This supports steadier overnight blood sugar, which may reduce those cortisol spikes.
If you want a straightforward guide focused on real-life menopause eating (energy, weight, and hormone balance), I recommend reading: Menopause nutrition: what to eat for energy, weight & hormone balance.
2) Trial a small bedtime snack (if you suspect blood sugar dips)
This is not a rule for everyone, but for many women it is a game changer.
A good snack is protein + fibre or fat (not just a plain biscuit or toast on its own). For example:
| Bedtime snack idea | Why it can help | Menopause-friendly notes |
|---|---|---|
| Greek yoghurt with berries and a spoon of ground flaxseed | Protein plus fibre, supports steadier blood sugar | Flax also provides phytoestrogens |
| Oatcakes with peanut butter | Carbs plus fat slows digestion | Choose unsweetened nut butter |
| Small bowl of porridge made with milk or soy milk | Gentle carbs plus protein | Soy milk adds extra protein and phytoestrogens |
| A kiwi fruit plus a small handful of nuts | Fibre plus healthy fats | Keep portions small to avoid reflux |
If reflux is an issue for you, keep snacks small, finish at least 60 to 90 minutes before bed, and prop the head of your bed slightly.
3) Support temperature regulation
Simple tweaks can make a surprising difference:
- Keep the bedroom cool (many women sleep best around 16 to 18°C)
- Use breathable bedding and layers you can peel off
- Consider a cool shower in the evening if you run hot
- Limit alcohol, which can worsen night sweats and sleep fragmentation
Hydration matters too, but you do not want to be up all night weeing. Aim to front-load fluids earlier in the day and sip in the evening.
4) Get daylight early, dim light late
Your body clock is heavily influenced by light.
- Try to get outside light within an hour of waking, even if it is cloudy.
- In the evening, dim lights and reduce screen glare where you can.
This supports melatonin rhythm and may help with those “tired but wired” nights.
Nutrition that supports sleep in menopause (without being restrictive)
Sleep and weight changes often travel together in menopause. Poor sleep increases hunger hormones and cravings, and it can make weight management feel much harder, even when you are eating well. This is one reason many women seek support from a weight management nutritionist at this stage, not for a harsh diet, but for a plan that supports sleep, appetite, and energy together.
Here are the nutrition focuses I come back to again and again.
Prioritise protein earlier in the day
Many women are unintentionally under-eating protein at breakfast and lunch, then getting snacky later. A protein-forward morning meal can support steady energy and fewer cravings.
If you want a practical way to work out your target, you might find my site’s protein calculator helpful.
Magnesium-rich foods (and when supplements might be worth considering)
Magnesium supports nervous system regulation and muscle relaxation, and low intakes are common.
Food sources include:
- Pumpkin seeds, nuts, and cacao
- Beans and lentils
- Leafy greens
- Wholegrains
If you are considering supplements, quality and dose matter, and it is important to check suitability with your GP or practitioner if you take medication. I also keep a page of trusted resources and recommendations here: Useful links and resources.
Support gut health gently
Your gut and brain are in constant communication. If digestion is off (bloating, reflux, constipation), sleep can suffer.
A simple place to start is a consistent meal pattern, more plant variety, and slowing down when you eat.
When should you get extra help?
If insomnia is happening most nights for more than a few weeks, or it is affecting mood, work, relationships, or your confidence around food, it is worth getting support.
Options to discuss with your GP may include:
- Menopause treatment options (including HRT, if appropriate)
- CBT for insomnia
- Screening for sleep apnoea, thyroid issues, iron deficiency, or anxiety
From a nutrition and lifestyle perspective, personalised support can help you identify what is driving your pattern (stress hormones, blood sugar, gut health, meal timing, nutrient gaps) and create a plan that fits your real life.
A quick “tonight” plan if you wake at 3am
If you are reading this at 3:07am, try this:
- Keep lights low and avoid checking the time repeatedly
- Do 2 to 3 minutes of slow breathing (longer exhale than inhale)
- If you are hungry, try a small protein-based snack (see table above)
- If you are hot, cool down first (layers off, sip of water, cool pack near feet)
- If you are awake more than 20 to 30 minutes, consider getting up briefly and doing something calming in dim light, then return to bed when sleepy
Frequently Asked Questions
Is waking at 3am a sign of low oestrogen? It can be related, but it is rarely just one hormone. In menopause, sleep disruption is often a mix of temperature changes, cortisol rhythm, mood, and blood sugar stability.
What is the best supplement for menopause insomnia? There is no single best supplement for everyone. Magnesium can be helpful for some women, and other options may be appropriate depending on symptoms and medications. It is always best to personalise this with your GP or a qualified practitioner.
Can menopause insomnia cause weight gain? Poor sleep can increase appetite, cravings, and fatigue, which can make weight management harder. Supporting sleep often helps eating feel more steady and less effortful.
Should I eat if I wake up at 3am? If your waking is driven by hunger or blood sugar dips, a small protein-based snack can help some women fall back asleep. If you suspect reflux, keep snacks minimal and review evening meal timing.
When should I see my GP about insomnia in menopause? If insomnia is persistent, severe, linked to low mood or anxiety, or you have symptoms like snoring/gasping at night, chest pain, or significant daytime sleepiness, it is worth speaking to your GP.
Want help figuring out what’s driving your sleep?
If you’re in perimenopause or menopause and sleep is becoming a nightly battle, you do not have to troubleshoot it alone. I offer personalised, whole-food nutrition support (in Nantwich, Cheshire and via video call nationwide) and a free 15-minute consultation so you can talk things through and see what kind of support would be most helpful.
You can book a chat or get in touch via Tracey Warren Nutrition.




